By Morgan Faith
Photographs by Mike Confer
Nursing students are preparing to thrive in a demanding field with a collaborative learning model focused on mastery, inquiry, and empathy.
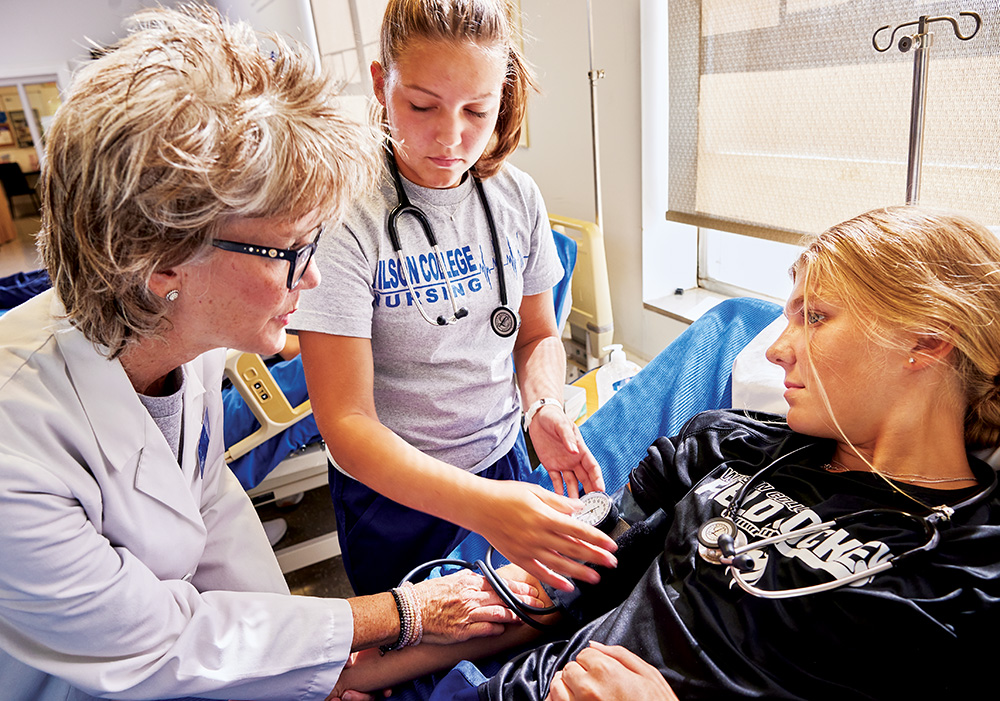
A young woman in scrubs and a Wilson Athletics T-shirt rubs imaginary sanitizer into her hands as she walks toward her patient, who is lying in a standard hospital bed. “How are you feeling today? Are you in any pain?” she says, and her patient replies amidst the murmur of other students going through the same exercise.
This is 20 nursing students’ first day in the clinical classroom at Wilson College. Their assignment, following nursing instructor Sherri Stahl’s 20-minute lecture and discussion, is to conduct a head-to-toe intake assessment on one another: Look at the color and condition of the skin, take vital signs including temperature and blood pressure, understand any pain they report. And importantly, Stahl emphasizes, get to know the patient and let them know the nurse is there for them.
“The people you see are in pain, they have concerns, they have family who want to know what’s going on. It goes such a long way when you let them know that everything you do, you’re doing for them,” says Stahl.
Importantly, the students are putting ideas and information into practice immediately after taking it in. And the connection of these two learning principles – human connection and clinical practice from literally day one of learning – are setting Wilson nursing students apart.
Addressing the need for qualified nurses
Since the COVID-19 pandemic in 2020, an increasing number of nursing staff shortages has affected healthcare facilities nationwide. The high-stress environment that healthcare professionals experience has caused more nurses to walk away from their jobs and put their mental and emotional health first. Those who stay often experience substantial job dissatisfaction, burnout, and workplace conflict.
“Burnout is a real thing, and it’s bad,” says Kim Erwin, an instructor of nursing at Wilson College. She is currently working on a Ph.D. at West Virginia University investigating incivility among nursing students. At Wilson she brings cutting-edge teaching methodologies to the classroom, helping nursing students prepare for the high-stress environment that they will inevitably encounter each day. A recent study by the University of Pennsylvania School of Nursing found that poor staffing as a source of workplace stress was an issue even prior to COVID-19, reporting that nearly 65 percent of medical-surgical nurses felt their departments were insufficiently staffed before the pandemic. However, the study noted, reports of burnout rose to about 75 percent during the pandemic.
In response to the urgent need for educated nurses and physicians, hospitals have started their own training programs. In Franklin County and across south-central Pennsylvania, WellSpan Health launched its WellStaffed program mid-pandemic to place registered nurses and certified nursing assistants in healthcare facilities with the highest need. They also added 200 mental health practitioners to their staffs to address increased pandemic-related needs.
Elsewhere, says Mindy Guinard, Ed.D., Wilson’s interim director of nursing and health sciences, healthcare providers hired healthcare workers, some with little or no nursing experience, while training them with new in-house programs to become certified nurse assistants or licensed practical nurses. “That was an important step in response to a dire need, but the result is that now we have an increase in CNAs and LPNs who are going back to school for their RN,” she says. The registered nurse qualification is a more rigorous program and is preferred by most healthcare providers.
The way Guinard sees it, this creates a significant opportunity for Wilson College: Combine the nurturing, human-focused culture we’re known for with the most innovative nursing education available to train nurses to have the academic knowledge, technical expertise, mental agility, and interpersonal skills to meet the unique and considerable demands of today’s healthcare environment. An important part of the nursing program’s mission is to produce nurses who are better prepared for the clinical, mental, and emotional curveballs that come with being a nurse.
Open doors, small classrooms
At Wilson, the nursing program enrolls students with a variety of experiences in the field. From high school graduates with zero experience to LPNs and CNAs with several years of experience, the Wilson nursing program accepts each student as they are. Many traditional university nursing programs, by contrast, can require up to two years of preparatory courses before starting any clinical training.
This can create a number of challenges, Erwin says. First, students can invest years in a career objective but end up realizing it’s not for them when they begin clinical training. Second, the time spent almost exclusively in the classroom can instill excellent study and memorization habits that do not translate well into the field.
At Wilson, the experience is quite different. The nursing curriculum stretches over four years rather than two – and hands-on clinical practice begins on day one. Students have a chance to truly hone their critical thinking and clinical judgment skills, develop connections with professors, and prepare more realistically for the pressures of nursing – with the freedom to make mistakes.
The perfectionism problem
In nursing, Erwin explains, students and professionals alike commonly struggle with perfectionism. In some of her clinical labs, Erwin says, students don’t always aim to fix problems that arise mid-procedure. “They stop and want to start from the beginning,” she says. “That’s not an option with a real patient. So we practice how to handle that situation in the moment.” Instead of walking away, giving up on trying to solve the problem, students learn to turn off the perfectionistic mindset that halts thinking and work through what they can do to help the patient.
“As nurses, we were always told there were two right answers – sometimes more. Your job as a nurse is to pick the best one,” Erwin says. “What are your other options? We don’t go back to the beginning. We start where you ended and keep going.” Wilson nursing students learn to consult with their teachers and colleagues, ask for help, and use their clinical judgment skills in real time.
 Instead of teaching students that a mistake can’t be fixed, the instructors at Wilson are teaching them that it is OK to make mistakes and be wrong. “A failure is not in making a mistake,” Erwin says. “A real failure is to recognize the problem, ignore your mistake or pretend it didn’t happen, and not try to solve it.”
Instead of teaching students that a mistake can’t be fixed, the instructors at Wilson are teaching them that it is OK to make mistakes and be wrong. “A failure is not in making a mistake,” Erwin says. “A real failure is to recognize the problem, ignore your mistake or pretend it didn’t happen, and not try to solve it.”
A more effective pedagogy, Erwin says, is taking the pressure off of the learner and encouraging the instructor to guide, give feedback, and allow students to experience more hands-on learning. Nursing is one of those professions that requires a high level of skill in physical activities performed in settings that can be very high pressure and unpredictable – not unlike being a professional athlete, she says. This requires repetition in an atmosphere of acceptance and encouragement. Currently, the nursing staff are helping students change their perfectionism to a more open mindset of growth, learning, asking questions, and asking for help.
“A mistake is not a failure,” Stahl reminds students in her class, echoing Erwin’s sentiments. “It’s not a setback. It’s a chance to think through your available options.”
Mastery over memorization
These are not the kinds of skills that can be mastered strictly by memorizing medical terminology and standard operating procedures. In fact, Erwin says, relying solely on memorizing information is an approach to learning that actually interferes with true mastery, which she aims to instill in students.
And although Wilson’s program does lead with innovative principles of nursing education, it is not unique.
The NCLEX exam, the standard test of nursing competencies in the United States and Canada, has shifted in recent years to a test design that evaluates nurses’ clinical judgment, critical thinking, and overall ability to apply knowledge in a variety of scenarios. Wilson graduates’ NCLEX scores have been steadily increasing since 2021. Erwin and Guinard attribute students’ test performance, among other things, to their growing ability to take tests that are designed this way, as opposed to a traditional multiple-choice
format that tests knowledge removed from application.
Wilson’s program is on the small side, and in this regard that is an advantage. Instructors get to know students well, and students get significantly more attention and clinical practice time than they might in a larger program.
Historically, memorization has always been a huge part of learning. Classrooms even today feature overhead projectors, PowerPoint presentations, long lectures, and readings that students are expected to prepare and discuss in class. However, instructors like Erwin have stepped away from the big projectors and long lectures. “We are teaching the process of how to act on a patient,” she says. “That is not
a passive exercise.” Nursing classrooms at Wilson comprise two sections: a set of tables that seat two students per desk and two rows of standard hospital beds, as well as a supply of medical equipment such as IV stands, monitors, and the like. Rather than learning how a nurse would potentially, in their imaginations, interact with a new patient or react to saving a life, students spend time in an actual nurse’s shoes.
In one recent class, first-year students sat down for a 20-minute lecture and discussion on initial patient assessments led by Sherri Stahl with Associate Professor Jennifer Buffenbarger assisting. There’s the typical back and forth as students raise their hands and offer knowledge they’ve learned from previous discussion, reading, and possibly firsthand professional experience. The class appears lively; the students seem curious; their faces light up when they hear a perspective they hadn’t considered before.
The growth mindset is baked into the teaching. “There’s nothing wrong with not knowing,” Stahl says, preparing the class for the clinical roleplay they’re about to start. “What you have to do is develop the skill to say, ‘Let me check, so I can give you the best information.’”
Moving on to the clinical portion of class, students pair up for intake assessments in which they practice
skills such as handwashing, greeting the patient, asking about pain, and taking the patient’s vitals. While it’s awkward at first, students soon embrace the experience – and discover just how much there is to learn in something as apparently simple as checking someone’s vital signs. Is the hospital bed the right height? How do I adjust it? Am I standing at an angle that is comfortable and safe for both the patient and myself? What’s the optimal position for a patient to be in to take a blood pressure reading? What is
my comfort level with touching people in a clinical setting? Right away, the number of variables to consider can be daunting.
The complexity and the value of this basic practice is not lost on students. First-year student Audrey Leke says, “I feel like these clinical labs give the experience of actually being in the patient’s shoes. Being in the patient’s place, you really understand the material more.”
As students practice, the instructors circulate, offering guidance and feedback. Mentorship is a critical aspect of learning success, says Buffenbarger. “As nurses, we treat the whole patient, the whole person, not just their symptoms or injuries,” she says. Holistic nursing, she continues, begins with the relationship between the nurse and the patient, and that begins with the relationships that are built between the instructors and students at Wilson.
Breaking down historical learning barriers
Over the course of just one decade, teaching and learning have progressed immensely. Erwin observes how the learning environment for students has changed. To Gen Zers in many education settings across the country, “plagiarism and cheating don’t exist,” she says. The new generation of students share information freely with one another. They give each other a heads-up about tough questions to look out for on a test.
This collaborative, supportive attitude can be helpful when studying for a traditional exam, and it certainly goes a long way toward creating a friendly, collegial working atmosphere. For anyone mastering skills that will be used out in the field, it can be misleading and even harmful, Erwin says.
In addition to leaving behind those PowerPoints and passive lectures, Erwin uses a variety of learning devices to mix things up and require students to demonstrate that they understand the information, not just that they have learned it superficially. One popular activity in her classes is a game that challenges students to explain a concept or procedure using plain language rather than dictionary definitions. She also sets up debates in class so that emerging nurses engage with one another and defend their arguments.
Students appreciate being more hands-on and interactive. “I feel more confident when I come into clinical practice after learning the material,” first-year student Hannah Bost says.
New nurses for a new era
Nursing education at Wilson and in many colleges is moving away from the typical lectures, stressful exams, and rote memorization and instead is giving students a chance to flourish in their degree program through hands- on experiences; empathetic, holistic care; and a radical growth mindset. But in a post-Covid era of continued understaffing, high stress, and competitive work environments, how will these innovative strategies prepare graduates to succeed when they’re out in the field?
Erwin reflects for a moment. “We may be small in number, but every one of the professors in this program is absolutely passionate about nursing and about creating nurses who capture our love of helping people as well,” she says.
No doubt, nursing is a high-stress profession that has caused many to walk away from their jobs. Helping students in Wilson’s nursing program learn, grow, and understand that they can make a positive impact on patients’ lives is something that the program’s faculty always aim to communicate.
Back in the first-year class, Sherri Stahl fits some coaching into her lecture on the first encounter with a patient. Nurses downplay their contribution sometimes, she says, and she encourages her students never to accept that kind of thinking. “Nurses are entrusted with human life, so you’re never just a nurse,” Stahl says. “It takes a nurse to save your life.”
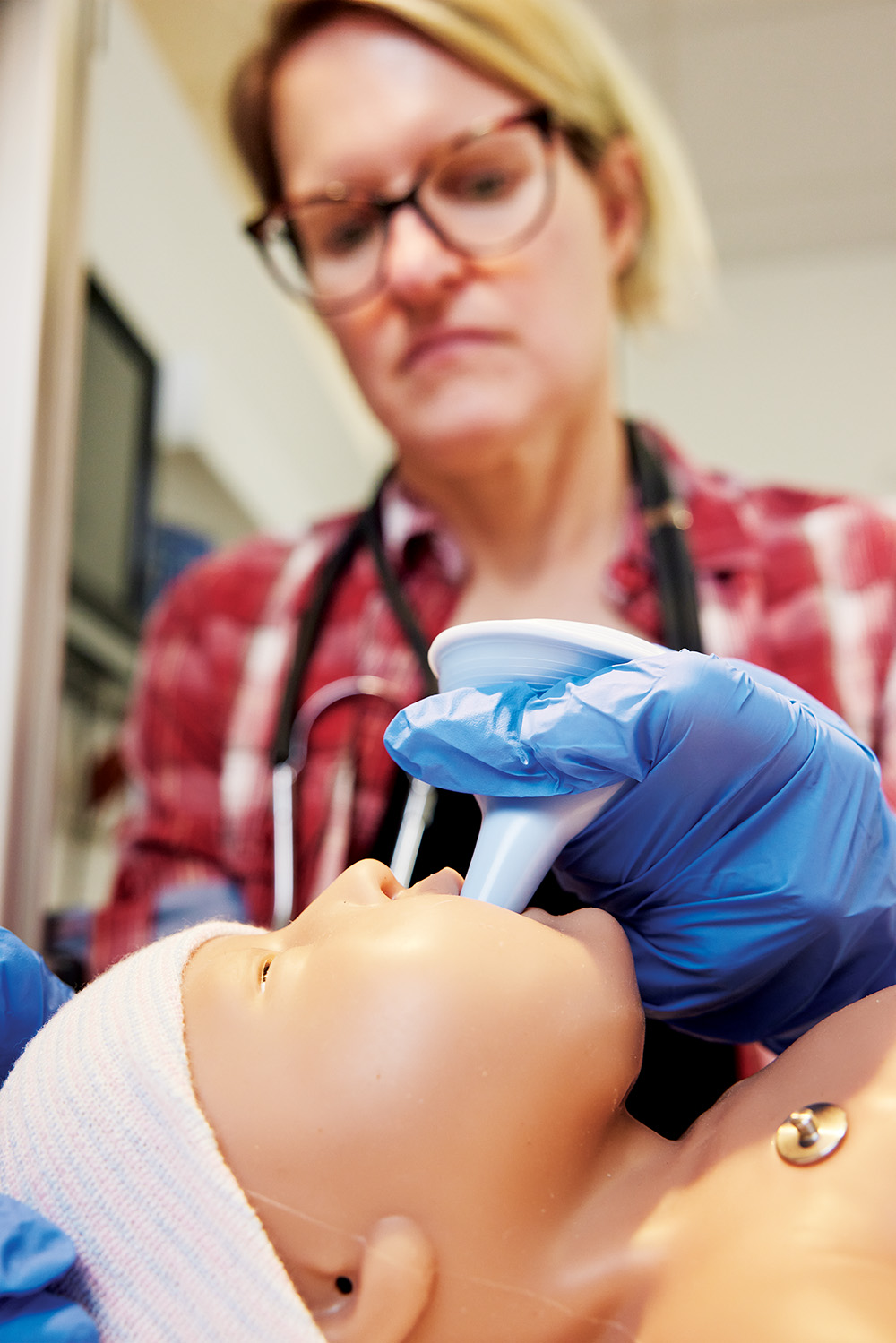
Sim Nursing
A secret weapon of many nursing and other healthcare programs worldwide, the simulation lab (sim lab) allows students to obtain lifelike clinical practice well before they start interacting with live patients. Wilson acquired its first avatars in 2016 and has been steadily upgrading. Today the lab holds 12 adult avatars, one young child avatar (Hal, acquired in 2020), and a state-of-the-art birthing mother (Noelle) and infant, purchased in 2022. Each sim patient can be connected to real equipment and monitors and programmed to present with a wide variety of issues, including cardiac events, stopped breathing, and more. Here, Instructor Kim Erwin, who specialized in pediatric nursing in her practice, demonstrates a standard neonatal checkup on Wilson’s sim baby. “Students start working with the avatars as early as possible, and we encourage them to book time outside of class to practice any procedure,” Erwin says.